5 July 2020
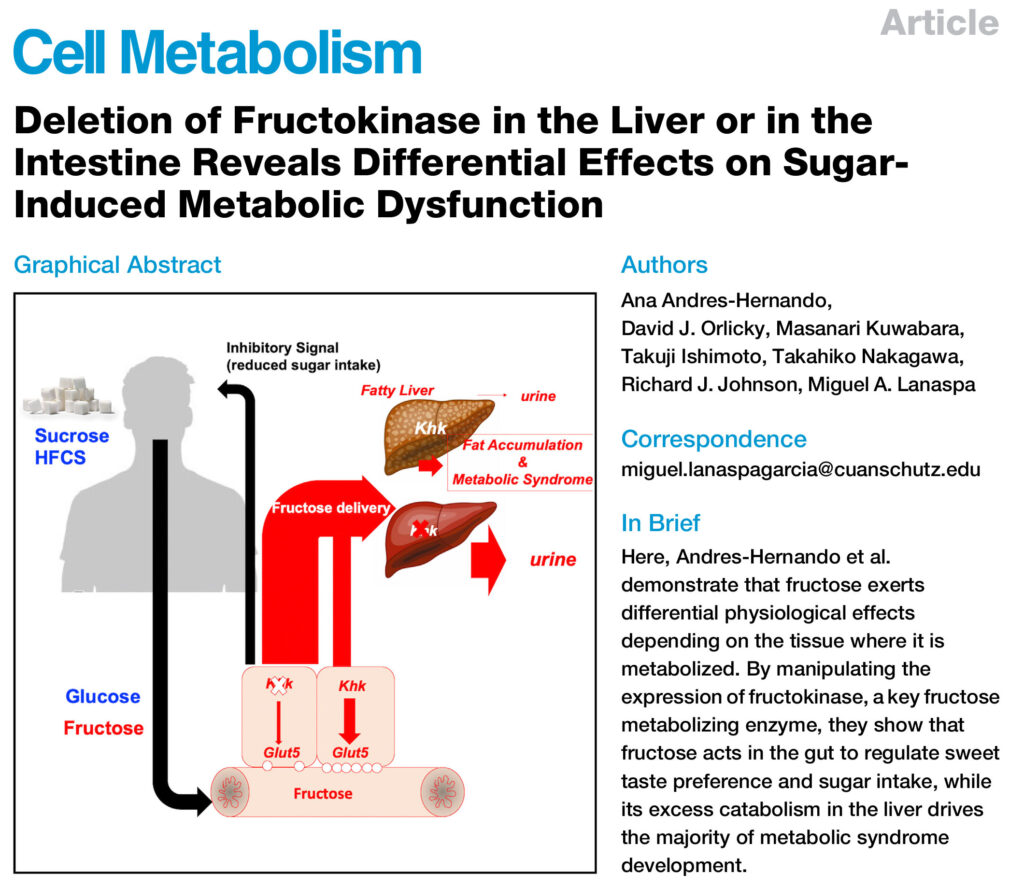
New Research: How bad is fructose for us?
Recently, I came across an interesting paper on fructose. Fructose is commonly taken in as table sugar, high-fructose corn syrup and also as fruits. Table sugar, or sucrose, is a dimeric sugar consisting to equal parts of glucose and fructose. High-fructose corn syrup, which is added to coke and other soft drinks, contains 55% fructose and 45% glucose.
First, some not-so-fun facts about fructose and sugar in general from Veronique Douard and Ronaldo Ferraris review on fructose transporters. Centuries ago, sugar used to be much more expensive. And so in 1700, Europeans consumed only about 5 grams of sugar per day. In 1950 it was 120 grams per day and today it is 180 grams per day on average. If we consider that 1 gram of sugar has 3.9 calories, then an average person consumes about 700 calories of sugar alone. That is about a third of the recommended calorie intake (which is 2000 calories for women and 2500 for men). So one can imagine how many calories we can save if we just stop to eat and drink sugar. One can of coke alone contains 39 grams of sugar, of which half is fructose.
There are some important differences between glucose and fructose. While glucose can be taken in and used by all cells in our body, fructose is only metabolized in the liver. This is because only the liver has the necessary transporters and enzymes to utilize fructose. (The intestine also expresses fructose transporter proteins in order to absorb fructose from the food to then be transported into the liver.) If we take in a lot of fructose with a meal or sugary drink, one can hence imagine that the liver as the only fructose-metabolizing organ is overwhelmed. The available fructose exceeds the needs of liver cells for energy production and hence, the liver cells are unable to utilize all the fructose. The excess fructose is converted into lipids, or fat, which ends up in the liver (as fatty liver) and other organs.
What is also different between glucose and fructose is that glucose metabolism is highly regulated. As a result, cells only take in glucose if they are in need of it, for instance to produce energy. Fructose metabolism, on the other hand, is not subject to such regulatory mechanisms. Hence, liver cells will continue to take up fructose beyond their needs, leading to more lipid accumulation.
Evolutionary, when our ancestors consumed lots of fruits, conversion of fructose into fat was a beneficial mechanism, because the stored fat allowed humans to survive during periods of food shortage. However, this survival mechanism has turned into a metabolic liability in modern times, where we consume vastly increased amounts of fructose.
In one of the papers published by Andres-Hernando et al. in Cell Metabolism in July this year, the authors looked at the role that fructose has on the sugar-induced metabolic syndrome. The metabolic syndrome comprises of a set of symptoms (central obesity, elevated fasting blood glucose concentrations, high blood pressure, elevated blood triglyceride concentrations, elevated blood cholesterol levels), and sugar increases all of them. The paper has a number of interesting findings:
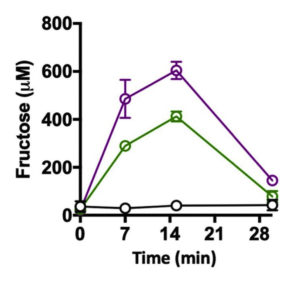
Firstly, the authors found that glucose stimulates fructose uptake (see the figure below). What that means is that the combination of glucose and fructose is particularly bad. (I initially thought that this may explain why fruits, which contain lots of fructose, are generally considered healthy. However, I realized that fruits also contain both fructose and glucose at a ratio of about 2:1. Hence, there must be other reasons why fruits are good for us despite being rich in sugar, which probably has to do with the high fiber content.)
Fructose levels in portal vein blood in mice after giving the mice water (black), fructose alone (green) or the same amount fructose together with glucose at an equal ratio (purple).
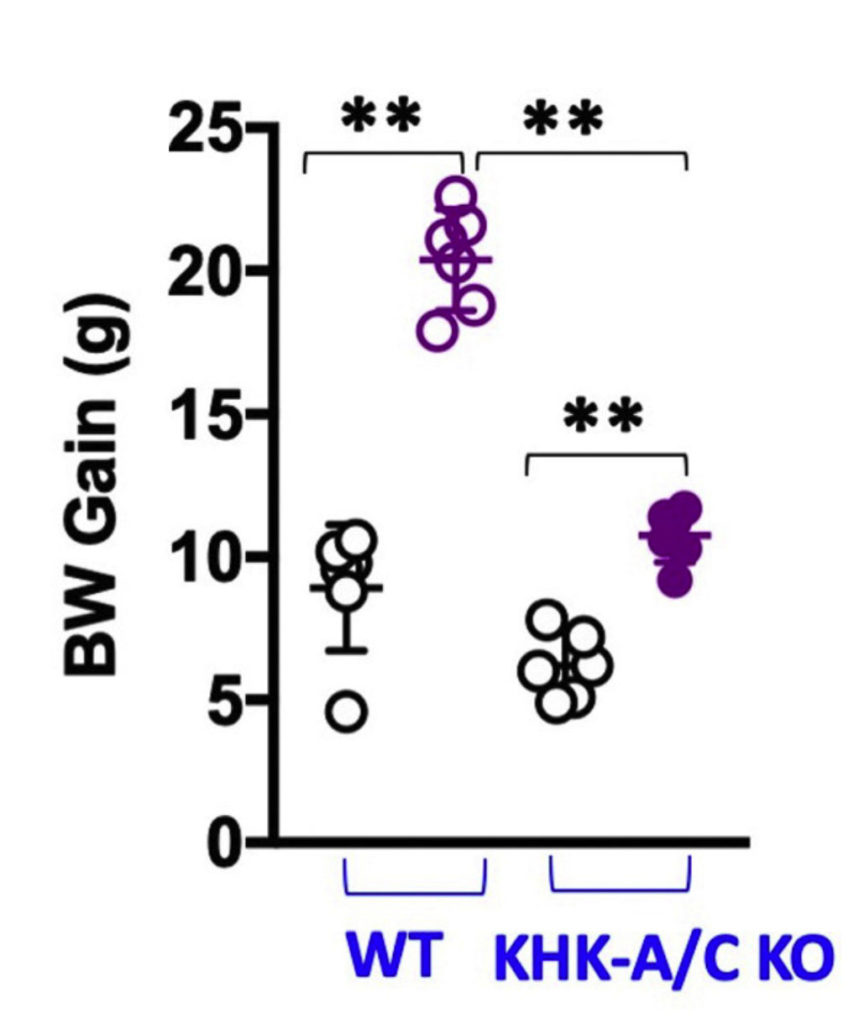
The authors then prevented fructose metabolism in cells. Fructose is normally taken up into cells via specific transporters. The first step in fructose metabolism is then the phosphorylation to fructose-1-phosphate, which is mediated by fructokinase. Fructokinase is also known as ketohexokinase (KHK) and exists as two separate isoforms, KHK-A and KHK-C. In the study, the authors knocked out both KHK-A and KHK-C. As a result, fructose metabolism and utilization is prevented. What the researchers found is that the KHK-A/C knockout mice, when exposed to high fructose+glucose diet, gained much less weight, showed less fat accumulation, did not develop fatty liver and maintained improved insulin sensitivity compared to the normal wild type mice. This means that it is actually the metabolism of fructose that is responsible for all the problems associated with sugar intake.
30-week body weight (BW) gain in normal wild type (WT) and fructokinase-deficient (KHK-A/C KO) mice exposed to water (black), 10% fructose + glucose (WT, purple open circles), or 30% fructose + glucose (KHK-A/C KO, purple closed circles). Fructokinase deficient mice gained much less body weight despite being exposed to more fructose + glucose.
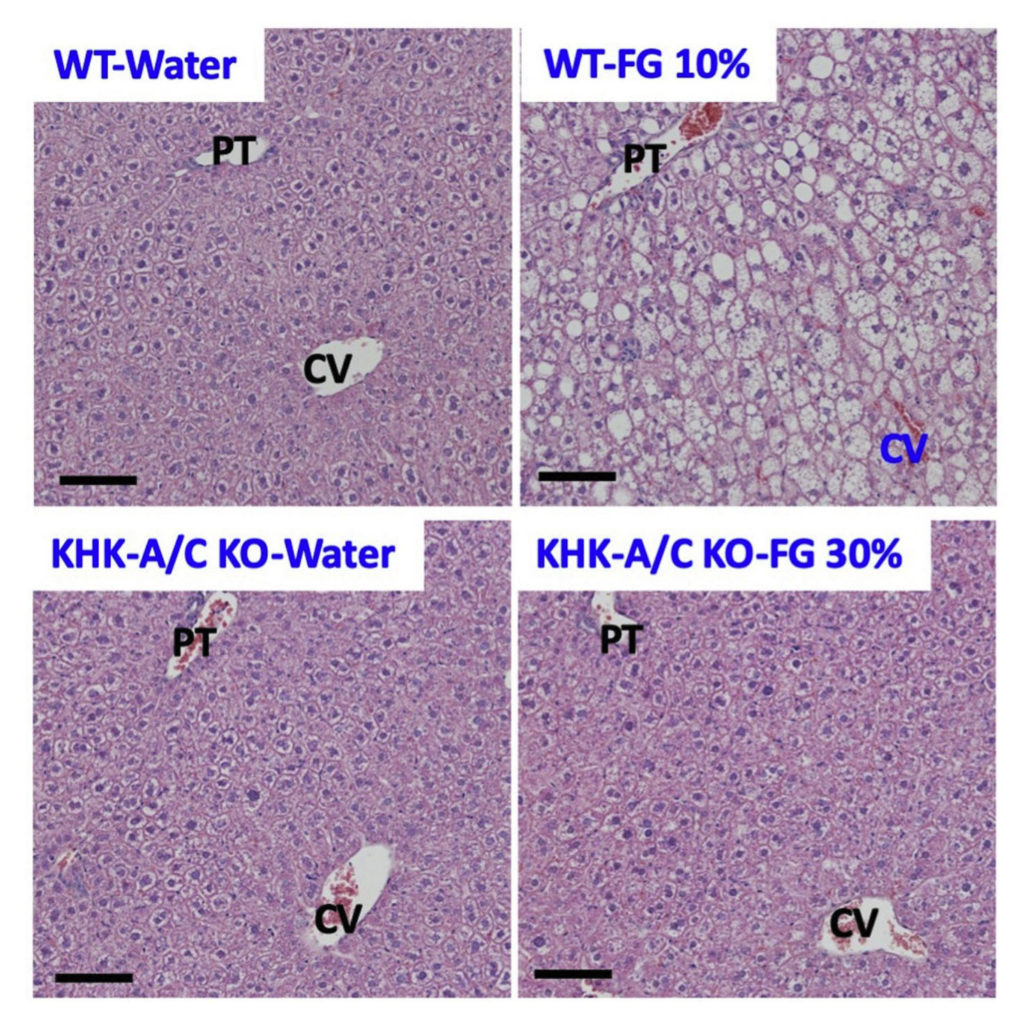
Representative histological staining (H&E) images of liver sections from normal wild type (WT) or fructose deficient (KHK-A/C KO) mice exposed to water or fructose + glucose (FG). Wild type mice develop fatty liver, as apparent from the accumulation of white lipid droplets. No lipid accumulation was observed in the liver of KHK-A/C KO mice. PT, portal triad; CV, central vein.
Mice lacking fructokinase actually took in less fructose via the gut. To compensate for this, in the experiments shown above the researchers actually gave 30% fructose + glucose to the fructokinase knockout mice, but only 10% to the wild type mice. To have a fairer comparison, the researchers then knocked out fructokinase only in the liver. As expected, this did not affect fructose uptake via the gut. Interestingly, despite the fact that fructose and glucose uptake is similar in wild type and liver-specific fructokinase knockout mice, absence of fructokinase in the liver completely protected mice from sugar-Induced metabolic syndrome. The mice lacking fructokinase in the liver did not show any increase in body weight, development of fatty liver, insulin resistance, increase in white fat and decrease in brown fat. The latter findings indicate that preventing fructose uptake in the liver even has effects on distant organs such as the adipose tissue.
Overall, the results suggest that when we take in sugar, the main problem is the metabolism of the fructose in the liver. Liver metabolism of fructose is responsible for all the problems associated with sugar intake. If metabolism of fructose in the liver is prevented, mice stay healthy. So staying away from fructose containing table sugar and high-fructose corn syrup in soft drinks is really a good idea.
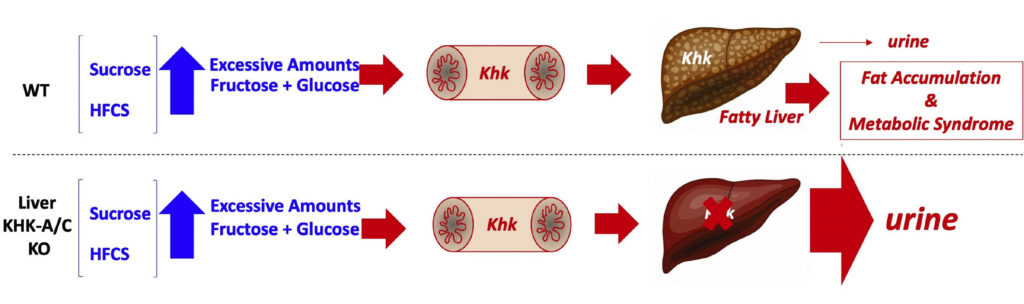
Excessive amounts of sugar (fructose and glucose) induce fatty liver and metabolic syndrome in normal WT mice by inducing greater sugar intake thus leading to increased fructose metabolism via KHK. The absence of KHK in the liver completely prevents fructose metabolism, leading to its excretion into the urine.
Interestingly, in another study the same group of researchers has previously shown that glucose by itself (without the addition of fructose) also causes signs of the metabolic syndrome in mice. In the study. the researchers provided mice for 14 weeks with drinking water containing 10% glucose (or tap water for the control mice), with an otherwise normal diet. For comparison, a can of coca cola contains 9 grams of sugar per 100 ml (9%). The authors found that glucose water caused a markedly increased body weight, increased fat accumulation (specifically accumulation of visceral fat) and elevated insulin concentrations (see figures below).
The researchers then tested the effect of blocking fructose metabolism. This was again done by using mice that lack fructokinase (also known as ketohexokinase = KHK-A/C), the first enzyme in the intracellular fructose metabolic pathway. Even more interestingly, and surprisingly, the effects of glucose on body weight, fat accumulation and insulin levels were, at least partially, blocked by preventing fructose metabolism.
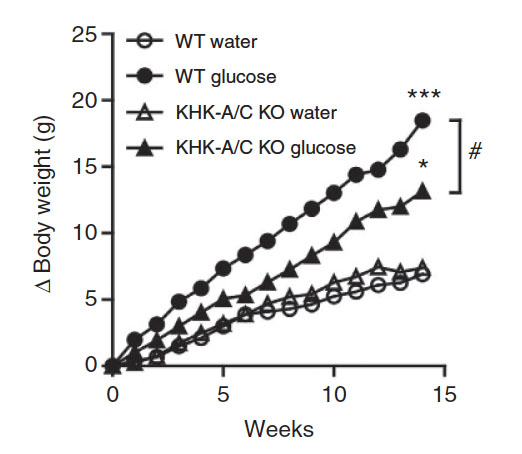
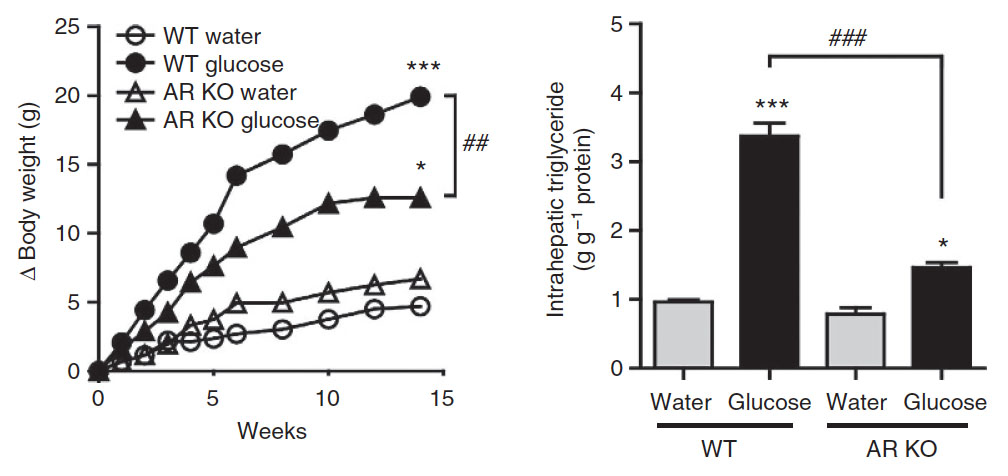
Effect of glucose consumption on body weight in normal wild type (WT) mice and mice that are unable to metabolize fructose (fructokinase or KHK-A/C knockout mice). The results show that in normal mice, drinking glucose water markedly increases body weight compared to drinking tap water. Inhibiting fructose metabolism partially inhibits the glucose-induced body weight gain.
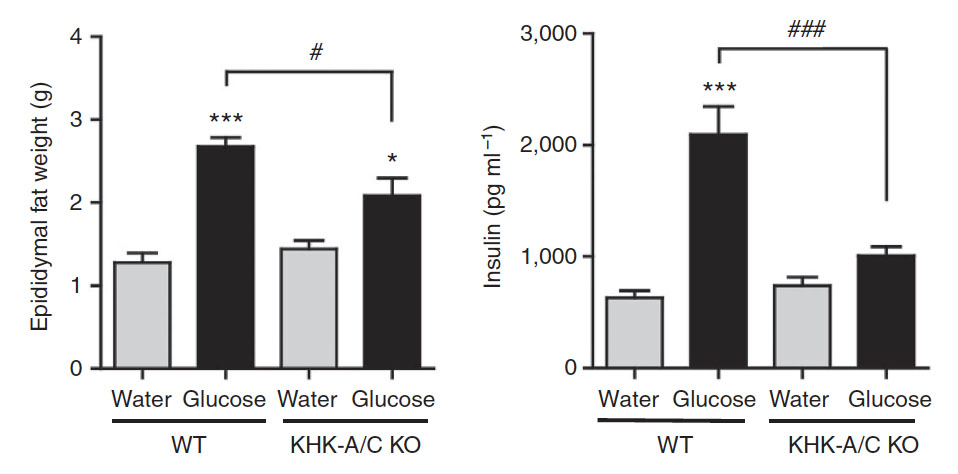
Normal wild type mice that drink glucose water have greater fat accumulation and insulin concentrations in the blood, indicative of insulin resistance. These effects are markedly inhibited when fructose metabolism is blocked in the KHK-A/C knockout mice.
In addition, glucose consumption also caused the development of fatty liver and elevated the amount of fat in the form of triglycerides in the liver (see figure below). Again, this effect was prevented if metabolism of fructose was blocked.
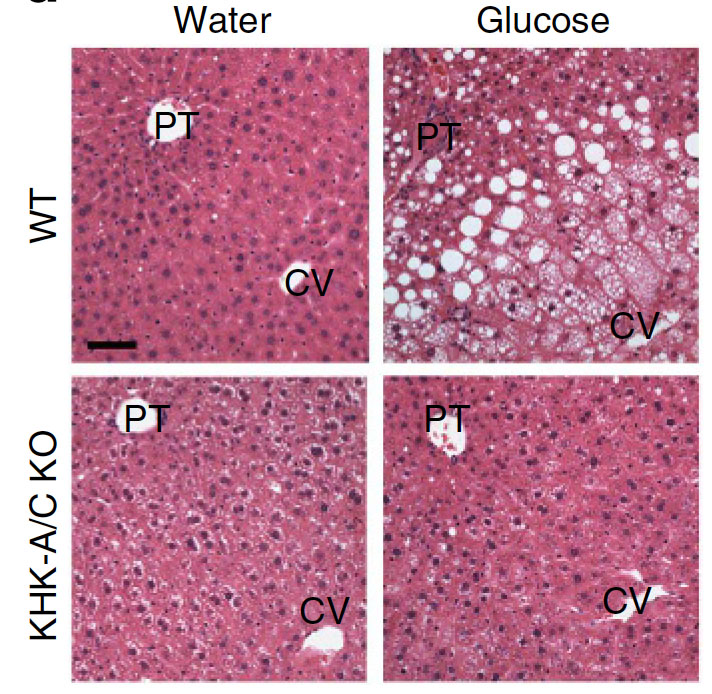
The figure shows that histological staining of liver sections. White lipid droplets accumulate upon consumption of glucose water in normal wild type mice but not in fructokinase deficient KHK-A/C knockout mice.
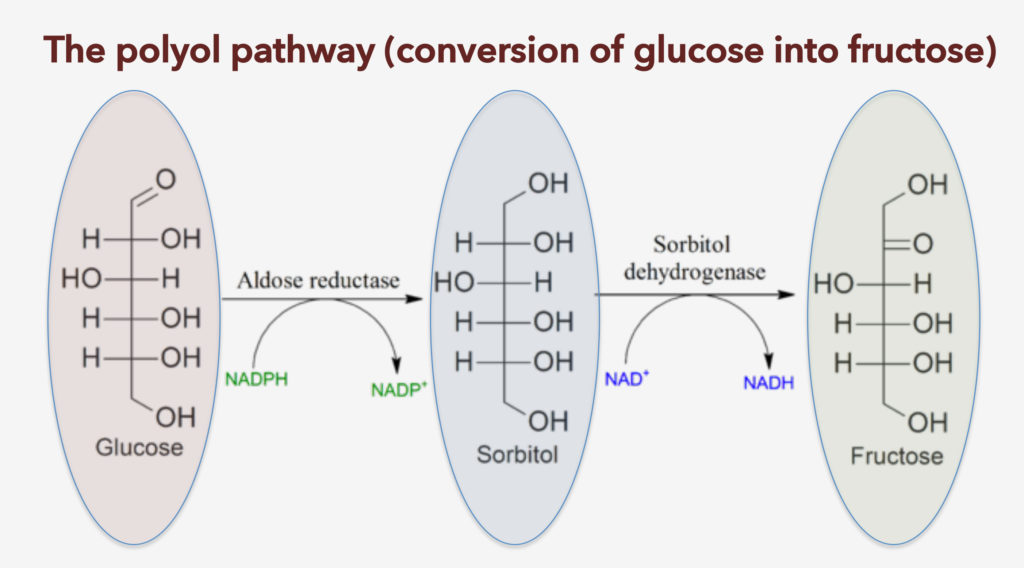
How can these unexpected findings be explained? It turns out that glucose can be converted into fructose via the so-called polyol pathway. Indeed, giving glucose to mice led to elevated fructose concentrations in the blood and liver. Importantly, preventing glucose conversion into fructose by knocking out the first enzyme of the polyol pathway, aldolase reductase, also inhibited body weight gain and fat accumulation in the liver upon giving mice glucose in their drinking water (see figure below).
Growth curves and liver fat (intrahepatic triglycerides) accumulation in normal wild type (WT) mice and mice that lack the enzyme aldolase reductase (AR knockout mice) and are unable to convert glucose to fructose via the polyol pathway.
In the polyol pathway, glucose is converted to fructose via two enzymes, aldolase reductase and sorbitol dehydrogenase. Interestingly, glucose was found to actually increase aldolase reductase (but not sorbitol dehydrogenase) activity, thus promoting its conversion to fructose.
The researchers have also shown that the metabolic effects of giving mice glucose water is not due to greater energy intake. Likewise, the protective effect of blocking fructose metabolism is also not due to lower calorie intake. These findings are important because they show that the harmful effects of glucose (and sugar in general) are not due to taking in more calories. Instead, glucose and fructose are harmful because they directly elicit damaging effects compared to more complex carbohydrates. These damaging effects are partly due to the very fast absorption of sugar and the resulting spikes in the blood sugar concentrations as well as the fact that fructose is only metabolized in the liver. In other words, if we take in sugar, it is the sugar itself and not the calories associated with it that cause the major health problems.
Nonetheless, it is important to keep in mind that the study was done in mice. Hence, it is currently not clear whether similar mechanisms operate in humans. However, the safest option is still to try to resist the temptation to eat too much sugar. This is how I managed to do it. But I subsequently discovered that a complete, lifelong commitment to abstinence approach works much better for me in most cases. This approach allowed me to make many other diet changes over the past five years.